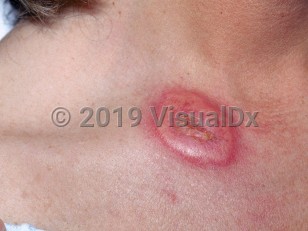
Acute febrile neutrophilic dermatosis, also known as Sweet syndrome, is an inflammatory disorder manifesting as multiple sterile, typically painful, edematous, erythematous plaques that are usually associated with fever and leukocytosis. The disease is typically limited to the skin, although any organ system may be affected. It is only rarely reported in children and infants, accounting for about 5% of all cases. In the pediatric population, the mean age of onset is 5 years, and there is a male predominance, particularly for children younger than 3 years. Sweet syndrome is classified by etiology:
- Classic idiopathic
- Pregnancy-associated
- Parainflammatory
- Paraneoplastic
- Drug-associated
A recent classification contracts this as follows:
- Classic (includes all inflammatory causes including infection, inflammatory bowel disease [IBD], and pregnancy)
- Paraneoplastic and drug-related
Pediatric Sweet syndrome is usually "classic" (total approximately 75%, with around 40% idiopathic and a third parainflammatory). About 25% are associated with malignancies. The predominant malignancies are hematologic in children. Drug-induced pediatric Sweet syndrome is less common. In terms of infection, pediatric Sweet syndrome is most commonly proceeded by an
upper respiratory tract or
gastrointestinal (GI) infection but has also been reported to follow
rotavirus infection,
tonsillitis,
otitis media, and
HIV infection. Parainflammatory Sweet syndrome in children can be seen in lupus (
systemic lupus erythematosus and
subacute cutaneous lupus erythematosus),
autoimmune hepatitis,
Crohn disease,
chronic granulomatous disease, primary T-cell immunodeficiency, and other primary immunodeficiencies. Paraneoplastic Sweet syndrome in children has been reported in
Fanconi anemia,
aplastic anemia,
osteosarcoma,
acute lymphocytic leukemia,
myelodysplastic disorder, juvenile
myelomonocytic leukemia, and
acute myelocytic leukemia. Drug-related Sweet syndrome has been reported from granulocyte colony-stimulating factor, trimethoprim-sulfamethoxazole, all-trans retinoic acid, and azathioprine.
Sweet syndrome can proceed a diagnosis of malignancy by several months.
Pediatric Sweet syndrome is categorized into:
- Neonatal Sweet syndrome (ages birth to 3 months).
- Infantile Sweet syndrome (ages 3 months to 3 years).
- Junior Sweet syndrome (ages 3-18 years).
Pediatric patients are less likely to report tenderness or pain compared to adults, and almost all pediatric patients will have leukocytosis, elevated erythrocyte sedimentation rate (ESR), and fever. Prodromal illness can be seen in just over one-half of cases. Arthralgia and arthritis are seen in over 20% of pediatric cases.
Pathergy is seen in up to a third of pediatric patients. Although still a minority of patients, it is slightly more common than in the adult population. When present, lesions will arise or worsen in sites of cutaneous injury, such as needle sticks. Fever may accompany or precede cutaneous involvement. The syndrome frequently includes extracutaneous manifestations such as fever, headaches, myalgias, malaise, arthralgias, and ocular inflammation. Other sites that may rarely be affected include the oral mucosa, liver (
hepatitis), kidney (
acute renal failure), lungs (pulmonary abscess and infiltrate), heart (
pericarditis,
aortitis), central nervous system (CNS) (
encephalitis), GI tract (
ileitis), lymphatics (lymphadenitis), musculoskeletal (myositis), and bones (sterile
osteomyelitis). Hypotension and tachycardia are rare but can occur as a result of systemic inflammation.
Although the exact etiology is still unclear, abnormal cytokine expression and atypical neutrophil function are thought to contribute to the pathogenesis. A genetic predisposition may also contribute.
Sweet syndrome typically responds dramatically to systemic corticosteroids, but recurrences can be seen in up to a third of cases.