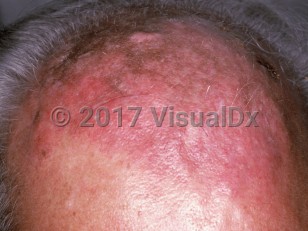
Angiosarcoma of skin
See also in: Cellulitis DDx,Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

Angiosarcomas are rare, aggressive, malignant neoplasms of vascular endothelial cell origin. They may arise in any organ or body site but have a predilection for skin and superficial soft tissues.
The most common form of angiosarcoma is cutaneous angiosarcoma (cAS). This may be primary, in which case it is most frequently located on the head or neck, particularly the scalp, of older individuals, more frequently men (ratio of 2:1); or secondary. In secondary cases, cAS develops in sites of chronic lymphedema or radiation exposure, and this subtype may be seen in a younger population. This type of cAS has also been termed lymphangiosarcoma.
Angiosarcomas grow rapidly, recur locally, and metastasize widely. Five-year survival rates of primary cAS range from 11%-50%. This is due to the biologic behavior of the tumor, delays in diagnosis, and poor impact on survival with currently available treatment options.
The appearance of angiosarcoma is highly variable. It may mimic ecchymosis or hematoma, cellulitis, rosacea, or facial edema, and this may lead to delay in diagnosis. The tumor or plaque may bleed or ulcerate after minor trauma and grow rapidly. Satellite nodules may be present.
Symptomatic thrombocytopenia (Kasabach-Merritt syndrome) has been seen in cases of angiosarcoma.
Pediatric patient considerations: Angiosarcoma is exceedingly rare in children and is more likely to be visceral than cutaneous. The prognosis is poor.
The most common form of angiosarcoma is cutaneous angiosarcoma (cAS). This may be primary, in which case it is most frequently located on the head or neck, particularly the scalp, of older individuals, more frequently men (ratio of 2:1); or secondary. In secondary cases, cAS develops in sites of chronic lymphedema or radiation exposure, and this subtype may be seen in a younger population. This type of cAS has also been termed lymphangiosarcoma.
Angiosarcomas grow rapidly, recur locally, and metastasize widely. Five-year survival rates of primary cAS range from 11%-50%. This is due to the biologic behavior of the tumor, delays in diagnosis, and poor impact on survival with currently available treatment options.
The appearance of angiosarcoma is highly variable. It may mimic ecchymosis or hematoma, cellulitis, rosacea, or facial edema, and this may lead to delay in diagnosis. The tumor or plaque may bleed or ulcerate after minor trauma and grow rapidly. Satellite nodules may be present.
Symptomatic thrombocytopenia (Kasabach-Merritt syndrome) has been seen in cases of angiosarcoma.
Pediatric patient considerations: Angiosarcoma is exceedingly rare in children and is more likely to be visceral than cutaneous. The prognosis is poor.
Codes
ICD10CM:
C49.9 – Malignant neoplasm of connective and soft tissue, unspecified
SNOMEDCT:
254794007 – Angiosarcoma of skin
C49.9 – Malignant neoplasm of connective and soft tissue, unspecified
SNOMEDCT:
254794007 – Angiosarcoma of skin
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:08/16/2023
Last Updated:09/24/2023
Last Updated:09/24/2023
Angiosarcoma of skin
See also in: Cellulitis DDx,Hair and Scalp