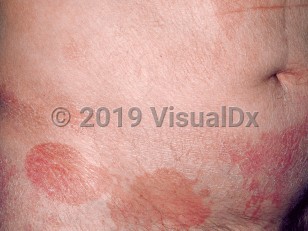
Cutaneous T-cell lymphoma in Child
See also in: Nail and Distal DigitAlerts and Notices
Important News & Links
Synopsis

The definitive diagnosis of CTCL may require large or multiple biopsies as well as specialized testing of the biopsy specimens. Typing of the CTCL and staging are important to determine the extent of disease and treatment strategy.
Mycosis fungoides and its variants (folliculotropic mycosis fungoides, pagetoid reticulosis, and granulomatous slack skin), Sézary syndrome, lymphomatoid papulosis, and cutaneous anaplastic large cell lymphoma make up 90% of all CTCL cases.
This summary focuses on mycosis fungoides and variants and Sézary syndrome.
Other types of CTCL discussed separately include subcutaneous panniculitis-like T-cell lymphoma, adult T-cell leukemia / lymphoma, and nasal type extranodal NK/T-cell lymphoma.
Mycosis Fungoides
Mycosis fungoides (MF) is the most common type of CTCL, accounting for 50% of all primary CTCL cases. Erythematous patches and plaques with fine scale and tumors that anatomically favor the buttocks and sun-protected areas of the trunk and limbs characterize this subtype. The etiology remains unclear. Current hypotheses propose that persistent antigenic stimulation occurs and that CD8+ T-cells play a critical role. MF takes on an indolent course over years to decades. Associated features include pruritus, poikiloderma in the patch stage, and ulceration of tumors. Poikilodermatous MF, a variant of patch stage MF, was seen in a higher percentage of children than has been reported in adults in one study. Extracutaneous involvement correlates with generalized skin involvement and erythroderma. Neoplastic T-cells demonstrate a memory T-cell phenotype: CD3+, CD4+, CD45RO+. MF staging requires CTCL physician specialists. Some consider large plaque parapsoriasis to be early patch stage MF.
Hypopigmented MF – A hypopigmented variant of MF is seen primarily in individuals of African descent but has also been reported in those of Asian, Indian, and Latin American descent. The hypopigmented variant is the most common form seen in childhood, accounting for over half of cases. The average age of diagnosis is 17 years.
Folliculotropic MF – This is characterized by lesions on the head and neck clinically and follicular involvement ("folliculotropism") microscopically. Most cases are seen in adult males, but children and adolescents may also be affected. It is the second most common variant in childhood. Early stage (IA, IB) disease with patches and plaques with follicular accentuation and keratosis pilaris-like or acneiform lesions may exhibit better prognosis with an indolent course. These lesions have a predilection for the trunk and extremities. On the other hand, advanced stage (IIB) disease with indurated or infiltrative alopecic plaques and tumors may be more aggressive with poorer prognosis. These lesions favor the head and neck and are more pruritic. 5-year survival rate approaches 80%.
Pagetoid reticulosis – Pagetoid reticulosis, also known as Woringer-Kolopp disease, is rarely reported in childhood. It represents approximately 1% of all cases of CTCL. It is a localized variant of MF, characterized by a solitary, slow-growing patch or plaque on a distal extremity clinically and striking epidermotropism microscopically. Pagetoid reticulosis has a predilection for middle-aged males but it can be seen in any age group. Prognosis is excellent with a 100% 5-year survival rate.
Ketron-Goodman disease is a disseminated and aggressive variant of pagetoid reticulosis with a potential for systemic involvement.
Granulomatous slack skin – Granulomatous slack skin, also known as granulomatous dermohypodermitis, is a rare variant of CTCL (<1% of all cases) that is very rarely seen in childhood. It is characterized by asymptomatic pendulous loose skin masses in the body folds clinically, and granulomatous T-cell infiltration microscopically. The disease may be associated with a lymphoproliferative disorder, such as MF, Hodgkin lymphoma, and non-Hodgkin lymphoma. Males in the third and fourth decades are more commonly affected. Overall, prognosis is good with a 100% 5-year survival rate.
Sézary Syndrome
While erythrodermic MF has been reported in childhood, true Sézary syndrome has not.
Codes
C84.A0 – Cutaneous T-cell lymphoma, unspecified, unspecified site
SNOMEDCT:
400122007 – Primary cutaneous T-cell lymphoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
 Patient Information for Cutaneous T-cell lymphoma in Child
Patient Information for Cutaneous T-cell lymphoma in Child- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient