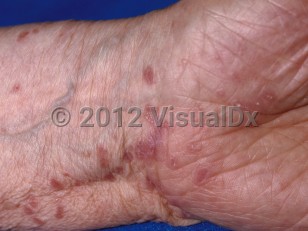
Lichen planus in Adult
See also in: Anogenital,Nail and Distal DigitAlerts and Notices
Important News & Links
Synopsis

Clinically, patients present with pruritic, flat-topped, pink to purple papules that are localized most commonly along the volar wrists, shins, presacral area, and hands, but may be widespread. Oral LP and/or LP involving the genitalia can occur in isolation or in patients with cutaneous disease. Lichen planopilaris, a variant of LP affecting the follicular unit, presents with perifollicular erythema and scaling and leads to scarring alopecia. (Frontal fibrosing alopecia is a variant that is seen in older women. Another rare variant is the Graham-Little-Piccardi-Lassueur syndrome.) LP can also affect the nail matrix, resulting in fissuring, longitudinal ridging, and lateral thinning of the nails.
Certain medications cause an LP-like eruption. Culprits include captopril, enalapril, labetalol, propranolol, methyldopa, calcium channel blockers, NSAIDs, chloroquine, hydroxychloroquine, quinacrine, thiazide diuretics, etanercept, infliximab, penicillamine, quinidine, and gold salts.
LP has been described in association with hepatitis C, predominantly in certain geographical areas (Japan and Mediterranean regions). Hepatitis B vaccination as well as exposure to other bacteria and viruses has also been associated with LP in the literature. Oral LP may occur on mucosal surfaces apposed to amalgams and other dental restorative materials.
Codes
L43.9 – Lichen planus, unspecified
SNOMEDCT:
4776004 – Lichen planus
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:05/12/2019
 Patient Information for Lichen planus in Adult
Patient Information for Lichen planus in Adult- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient