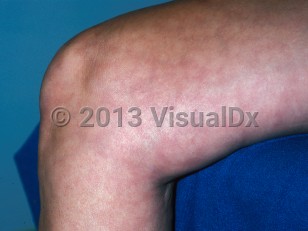
Livedo reticularis in Child
Alerts and Notices
Important News & Links
Synopsis

Cutis marmorata (CM) is a transient, benign (physiologic) presentation of LR that may also be seen in pale, gravid females.
Congenital LR, known as cutis marmorata telangiectatica congenita (CMTC), presents with persistent LR that can involve the trunk or extremities. Generally, the mottled discoloration is limited to one extremity but can be more generalized. There may be a sharp demarcation at midline with truncal involvement. CMTC is sporadically inherited (or autosomal dominant) and can be associated with limb, facial, and spine anomalies along with cutaneous atrophy. The vascular changes of the skin may improve during the first few years of life and resolve completely in approximately 20% of children with CMTC.
Many inherited vascular malformation syndromes are associated with CM or LR. LR is also associated with a host of other factors including anticardiolipin antibodies. It is seen with collagen vascular diseases such as Raynaud disease, systemic lupus erythematosus, dermatomyositis, scleroderma, polyarteritis nodosa, and temporal arteritis. In severe cases, the extremities are cold and ulcers may form.
Sneddon syndrome is extensive LR with central nervous system disease.
LR is also seen in patients with poor vascular flow due to peripheral vascular disease and cardiac failure, disseminated intravascular coagulation (DIC), deep vein thrombosis (DVT), vascular emboli, and vascular calcifications (in hypercalcemia). Infectious associations include syphilis, tuberculosis, streptococcemia, endocarditis, and rickettsial and viral diseases. Medication associations include amantadine, catecholamines, and quinidine; endocrine associations include hypothyroidism, pseudohypoparathyroidism, hypoparathyroidism, and Cushing syndrome.
Codes
R23.1 – Pallor
SNOMEDCT:
238772004 – Livedo reticularis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:09/03/2018
 Patient Information for Livedo reticularis in Child
Patient Information for Livedo reticularis in Child- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient