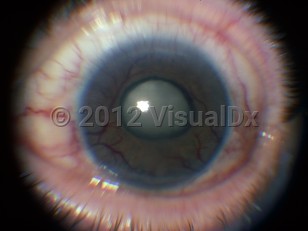
Neovascular glaucoma - External and Internal Eye
Alerts and Notices
Important News & Links
Synopsis

Patients with NVG typically present with acute or subacute loss of vision and severe eye pain. With very high intraocular pressures, the cornea is often hazy, making it difficult to detect neovascularization of the iris and angle. Prior to full development of NVG, patients can present without any symptoms but with neovascularization of the iris and/or angle on slit lamp examination and gonioscopy.
With poor circulation to the retina, new abnormal capillaries form from pre-existing vasculature. Vascular endothelial growth factor (VEGF) has become one of the most well-studied and key pro-angiogenic factors involved in angiogenesis. When VEGF stimulates angiogenesis of the iris and angle, the eye can develop NVG.
Proliferative diabetic retinopathy (PDR), central retinal vein occlusion (CRVO), and ocular ischemic syndrome are conditions most commonly associated with NVG. Other retinal ischemic diseases associated with NVG include central retinal artery occlusion, retinal detachment, Leber's congenital amaurosis, Coats' disease, Eales disease, sickle cell retinopathy, retinal hemangioma, persistent fetal vasculature, Norrie disease, Wyburn-Mason syndrome, carotid-cavernous fistula, dural shunt, Stickler syndrome, X-linked retinoschisis, Takayasu's aortitis, and juxtafoveal telangiectasis. Tumors of the iris, ciliary body, retina, choroid, and conjunctiva have been associated with NVG.
Sometimes procedures may contribute to NVG such as carotid endarterectomy, cataract extraction, pars plana vitrectomy, silicone oil implantation, scleral buckle, Nd:YAG laser capsulotomy, and radiation.
Rarely, inflammatory diseases have been associated with NVG, including uveitis, Vogt-Koyanagi-Harada syndrome, syphilitic retinitis, sympathetic ophthalmia, and endophthalmitis.
Codes
H40.89 – Other specified glaucoma
SNOMEDCT:
232086000 – Neovascular glaucoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required