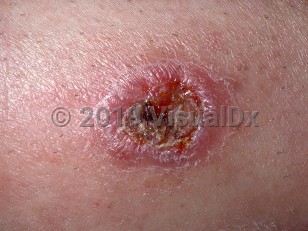
Cutaneous leishmaniasis in Child
Alerts and Notices
Important News & Links
Synopsis

Leishmaniasis is a disease caused by a protozoal parasite from over 20 Leishmania species distributed in different parts of the world. About 90 phlebotomine sandfly species are known to be vectors for Leishmania parasites. The parasites are transmitted through the bites of infected female sandflies, which feed on blood for egg production. About 70 animal species, including humans, can be the source of Leishmania parasites, although humans are incidental hosts of infection. Various mammalian reservoir hosts include dogs, rodents, opossums, bats, armadillos, and others.
Leishmaniasis is classified, based on the organ systems affected and the spectrum of clinical disease, into the following forms: visceral leishmaniasis (VL), cutaneous leishmaniasis (CL), and mucocutaneous leishmaniasis (MCL). This summary will focus on CL.
CL is the most common form of leishmaniasis and presents with one or more papules, nodules, or ulcers on mostly exposed parts of the body. Lesions can lead to lifelong disfigurement and scars and cause serious disability or stigma. About 95% of CL cases occur in the Americas, the Mediterranean basin, the Middle East and central Asia. It is estimated that 0.6 to 1 million new cases occur worldwide annually, but only around 200 000 are reported officially to WHO.
CL is most commonly caused by infection with Leishmania major, Leishmania tropica, and Leishmania aethiopica. Other species causing CL include Leishmania infantum and Leishmania donovani.
The incubation period generally ranges from 2 weeks or less to 2 months for CL.
Typically, the primary lesion starts as erythema at the site of a sandfly bite. Thereafter, it evolves, over weeks to months, from a papule to a nodule, which may then ulcerate with an elevated violaceous rim. Lymphangitis that ascends the lymphatic chain (sporotrichoid spread) and lymphadenopathy (sometimes bubonic) can be seen; the latter may precede the presence of skin lesions. Pruritus, pain, and bacterial superinfection may also be present. Systemic symptoms are rare.
Multiple primary lesions on one part of the body may be seen; this can result from the probing behavior of sandflies as they attempt to get blood meals. Multiple lesions are more commonly noted in individuals infected with L major than L tropica; up to 20 ulcers can be seen simultaneously in L major infection and fewer than 3 from L tropica. Ultimately, over weeks, months or years, lesions may heal without therapy, leaving hypopigmented, atrophic scars.
Chronic relapsing cutaneous leishmaniasis (leishmania recidivans) represents reactivation of infection. It is most commonly caused by L tropica and typically manifests as papules at the margins of scars, occurring months to years after clinical resolution of the initial ulcer.
Diffuse cutaneous leishmaniasis (DCL) is a rare variant caused by L aethiopica, L mexicana, and L amazonensis. It occurs in the context of leishmanial-specific anergy and is manifested by disseminated nonulcerated nodules and scars.
About Leishmaniasis
Leishmaniasis occurs in tropical and temperate regions restricted to natural habitats of the sandfly. In the World Health Organization (WHO) 2018 report, 92 countries were considered endemic for, or had previously reported cases of, CL. In 2022, the WHO estimated that more than 1 billion people live in leishmaniasis endemic areas and are at risk of acquiring infection. Annually, there are an estimated 30 000 new cases of VL, and more than 1 million new cases of CL occur. Leishmaniasis is on the WHO's list of neglected tropical diseases (NTDs). Children are more at risk to be infected with CL.
Approximately 95% of all CL and MCL cases occur in South America, the Mediterranean Basin, the Middle East, or Central Asia. In contrast, VL is more prevalent in Brazil, East Africa, and India. In 2018, over 85% of new CL and MCL cases reported to the WHO originated from Afghanistan, Algeria, Bolivia, Brazil, Colombia, Iran, Iraq, Pakistan, Syria, and Tunisia, while over 95% of new VL cases were reported in Brazil, China, Ethiopia, India, Iraq, Kenya, Nepal, Somalia, and Sudan. Four countries – Brazil, Bolivia, Ethiopia, and Peru – accounted for over 90% of new MCL cases.
In the Old World, infected humans may be the reservoir hosts for L tropica, which is anthroponotic and often endemic in urban areas. Recent periods of civil unrest and armed conflicts, with resultant poor sanitation and vector control, are some of the factors associated with ongoing epidemics of CL in Afghanistan and Iraq.
CL in the New World (America) is known by different names, based on the locality and clinical presentation: chiclero ulcer, forest yaws, bush yaws, uta, and pian bois. It is endemic in South America, Central America, and Mexico. More recently, acquired cases have been described in Texas, Oklahoma, and Florida.
In economically developed countries, infection is commonly associated with travel and immigration patterns. In the United States, for example, most cases of leishmaniasis are acquired outside the country. Individuals such as US travelers, government workers and volunteers, students, and military personnel are at risk of contracting the disease while overseas. Although sandflies can be found as far north as upstate New York, and cases of visceral leishmaniasis have been identified in foxhounds across various regions of the country, it is believed that human transmission is extremely rare in most of the United States. Occasional isolated cases of localized and diffuse CL have been reported in areas bordering Mexico, such as southern Texas and Oklahoma. While endemic leishmaniasis is uncommon in the United States, climate change may be altering patterns of acquisition. In Texas, for example, endemic leishmaniasis may be more common than travel-acquired disease due to more favorable environmental conditions for leishmaniasis vectors and reservoirs.
Leishmaniasis is classified, based on the organ systems affected and the spectrum of clinical disease, into the following forms: visceral leishmaniasis (VL), cutaneous leishmaniasis (CL), and mucocutaneous leishmaniasis (MCL). This summary will focus on CL.
CL is the most common form of leishmaniasis and presents with one or more papules, nodules, or ulcers on mostly exposed parts of the body. Lesions can lead to lifelong disfigurement and scars and cause serious disability or stigma. About 95% of CL cases occur in the Americas, the Mediterranean basin, the Middle East and central Asia. It is estimated that 0.6 to 1 million new cases occur worldwide annually, but only around 200 000 are reported officially to WHO.
CL is most commonly caused by infection with Leishmania major, Leishmania tropica, and Leishmania aethiopica. Other species causing CL include Leishmania infantum and Leishmania donovani.
The incubation period generally ranges from 2 weeks or less to 2 months for CL.
Typically, the primary lesion starts as erythema at the site of a sandfly bite. Thereafter, it evolves, over weeks to months, from a papule to a nodule, which may then ulcerate with an elevated violaceous rim. Lymphangitis that ascends the lymphatic chain (sporotrichoid spread) and lymphadenopathy (sometimes bubonic) can be seen; the latter may precede the presence of skin lesions. Pruritus, pain, and bacterial superinfection may also be present. Systemic symptoms are rare.
Multiple primary lesions on one part of the body may be seen; this can result from the probing behavior of sandflies as they attempt to get blood meals. Multiple lesions are more commonly noted in individuals infected with L major than L tropica; up to 20 ulcers can be seen simultaneously in L major infection and fewer than 3 from L tropica. Ultimately, over weeks, months or years, lesions may heal without therapy, leaving hypopigmented, atrophic scars.
Chronic relapsing cutaneous leishmaniasis (leishmania recidivans) represents reactivation of infection. It is most commonly caused by L tropica and typically manifests as papules at the margins of scars, occurring months to years after clinical resolution of the initial ulcer.
Diffuse cutaneous leishmaniasis (DCL) is a rare variant caused by L aethiopica, L mexicana, and L amazonensis. It occurs in the context of leishmanial-specific anergy and is manifested by disseminated nonulcerated nodules and scars.
About Leishmaniasis
Leishmaniasis occurs in tropical and temperate regions restricted to natural habitats of the sandfly. In the World Health Organization (WHO) 2018 report, 92 countries were considered endemic for, or had previously reported cases of, CL. In 2022, the WHO estimated that more than 1 billion people live in leishmaniasis endemic areas and are at risk of acquiring infection. Annually, there are an estimated 30 000 new cases of VL, and more than 1 million new cases of CL occur. Leishmaniasis is on the WHO's list of neglected tropical diseases (NTDs). Children are more at risk to be infected with CL.
Approximately 95% of all CL and MCL cases occur in South America, the Mediterranean Basin, the Middle East, or Central Asia. In contrast, VL is more prevalent in Brazil, East Africa, and India. In 2018, over 85% of new CL and MCL cases reported to the WHO originated from Afghanistan, Algeria, Bolivia, Brazil, Colombia, Iran, Iraq, Pakistan, Syria, and Tunisia, while over 95% of new VL cases were reported in Brazil, China, Ethiopia, India, Iraq, Kenya, Nepal, Somalia, and Sudan. Four countries – Brazil, Bolivia, Ethiopia, and Peru – accounted for over 90% of new MCL cases.
In the Old World, infected humans may be the reservoir hosts for L tropica, which is anthroponotic and often endemic in urban areas. Recent periods of civil unrest and armed conflicts, with resultant poor sanitation and vector control, are some of the factors associated with ongoing epidemics of CL in Afghanistan and Iraq.
CL in the New World (America) is known by different names, based on the locality and clinical presentation: chiclero ulcer, forest yaws, bush yaws, uta, and pian bois. It is endemic in South America, Central America, and Mexico. More recently, acquired cases have been described in Texas, Oklahoma, and Florida.
In economically developed countries, infection is commonly associated with travel and immigration patterns. In the United States, for example, most cases of leishmaniasis are acquired outside the country. Individuals such as US travelers, government workers and volunteers, students, and military personnel are at risk of contracting the disease while overseas. Although sandflies can be found as far north as upstate New York, and cases of visceral leishmaniasis have been identified in foxhounds across various regions of the country, it is believed that human transmission is extremely rare in most of the United States. Occasional isolated cases of localized and diffuse CL have been reported in areas bordering Mexico, such as southern Texas and Oklahoma. While endemic leishmaniasis is uncommon in the United States, climate change may be altering patterns of acquisition. In Texas, for example, endemic leishmaniasis may be more common than travel-acquired disease due to more favorable environmental conditions for leishmaniasis vectors and reservoirs.
Codes
ICD10CM:
B55.1 – Cutaneous leishmaniasis
SNOMEDCT:
402141004 – American cutaneous/mucocutaneous Leishmaniasis
B55.1 – Cutaneous leishmaniasis
SNOMEDCT:
402141004 – American cutaneous/mucocutaneous Leishmaniasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:07/15/2023
Last Updated:07/24/2023
Last Updated:07/24/2023