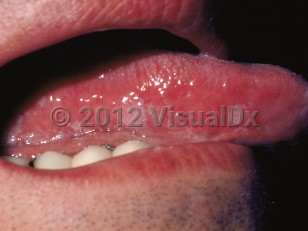
Oral hairy leukoplakia - Oral Mucosal Lesion
Alerts and Notices
Important News & Links
Synopsis

Hairy leukoplakia is a benign mucosal disorder caused by Epstein-Barr virus (EBV) infection and characterized by painless white plaques, typically on the lateral border of the tongue and often bilateral in distribution. The condition is almost always noted in immunocompromised patients.
It was first described in human immunodeficiency virus (HIV)-infected patients but is also seen in patients after organ transplantation. It may be associated with other immunosuppressive states like chemotherapy and hematological malignancies. Very uncommonly, the condition may affect otherwise healthy individuals, and it may be a more transient process in those patients.
The lesions of hairy leukoplakia are asymptomatic and do not scrape off, although they often have a superimposed candidal infection. Lesions develop over weeks to months.
It was first described in human immunodeficiency virus (HIV)-infected patients but is also seen in patients after organ transplantation. It may be associated with other immunosuppressive states like chemotherapy and hematological malignancies. Very uncommonly, the condition may affect otherwise healthy individuals, and it may be a more transient process in those patients.
The lesions of hairy leukoplakia are asymptomatic and do not scrape off, although they often have a superimposed candidal infection. Lesions develop over weeks to months.
Codes
ICD10CM:
K13.3 – Hairy leukoplakia
SNOMEDCT:
414952002 – Oral hairy leukoplakia
K13.3 – Hairy leukoplakia
SNOMEDCT:
414952002 – Oral hairy leukoplakia
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:12/17/2017
Last Updated:01/21/2018
Last Updated:01/21/2018