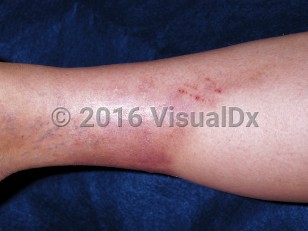
Panniculitis in Adult
See also in: Cellulitis DDxAlerts and Notices
Important News & Links
Synopsis

Erythema nodosum (EN) is by far the most common type of panniculitis and one of few mainly involving the septa (septal panniculitis). Other rarer types of panniculitis are generally classified as more lobular in nature and include infectious (necrotizing granulomatous) panniculitis, a panniculitis associated with systemic lupus erythematosus (lupus profundus), Weber-Christian disease, nodular vasculitis (erythema induratum), pancreatic panniculitis, cytophagic histiocytic panniculitis, and α1-antitrypsin deficiency panniculitis. There are also physical forms of panniculitis (cold panniculitis, factitial panniculitis). Furthermore, other diseases may be associated with a secondary panniculitis (necrobiosis lipoidica, polyarteritis nodosa, and some vasculitides).
EN is an inflammatory reaction pattern, sometimes precipitated by identifiable endogenous or exogenous stimuli. Streptococcal infections are the most common etiologic factor in children, while sarcoidosis, inflammatory bowel disease, and drugs are more commonly implicated in adults. Most cases are idiopathic. The eruption persists for 3–6 weeks and spontaneously regresses without scarring or atrophy. Fever with generalized aching sometimes accompanies the onset of skin lesions. EN can occur at any age, but most cases occur between the ages of 20 and 45. It is more common in women.
Panniculitis can be distinguished from cellulitis because it most often occurs bilaterally and lesions are often multifocal.
Codes
M79.3 – Panniculitis, unspecified
SNOMEDCT:
22125009 – Panniculitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required