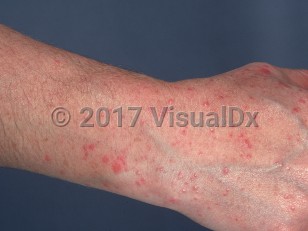
Polymorphous light eruption in Adult
Alerts and Notices
Important News & Links
Synopsis

Polymorphous light eruption (PMLE), or polymorphic light eruption, is a common acquired cutaneous disorder characterized by a pathological response to ultraviolet radiation (UVR). Erythematous papules, vesicles, and plaques (hence the name "polymorphous") develop minutes to hours after exposure to UVR, such as from sunlight or a tanning bed. The eruption is often pruritic, nonscarring, and photodistributed. Attacks most commonly occur during the spring and early summer months, especially after the first sun exposure of the season, and disappear during the winter. Systemic symptoms (such as fever, malaise, headache, myalgias, and arthralgias) are usually absent. While the eruption can last up to several weeks, most cases resolve within several days.
PMLE is most commonly seen in women with lighter skin phototypes aged 20-30 years, but it can occur in all sexes, ages, and ethnicities. Worldwide, prevalence is estimated to be from 10%-20%, with higher rates in higher altitudes and in Western countries. In a 2023 study of 844 patients, a significant proportion of individuals had darker skin phototypes, and further studies that elucidate prevalence in darker skin are needed.
The etiology of PMLE is not well understood. One theory is that UVR modifies antigens in the skin of PMLE patients to make them immunogenic. There are also data to suggest that PMLE involves a type IV delayed-type hypersensitivity reaction. The action spectrum for PMLE is UVA in most cases, but UVB and both UVA and UVB may also incite the response. Recent studies have shown that PMLE is associated with mutations in the NOD2 and TLR5 genes.
Although the condition frequently recurs, the tendency toward the development of PMLE and the severity of the eruption diminish with repeated sunlight exposure. This phenomenon is termed "hardening." As the summer proceeds, it has been observed that the incidence of new eruptions decreases. Prophylactic phototherapy supports this concept of hardening or tolerance.
Despite the variability of presentations, individual patients tend to experience the same clinical manifestations with each episode.
PMLE is most commonly seen in women with lighter skin phototypes aged 20-30 years, but it can occur in all sexes, ages, and ethnicities. Worldwide, prevalence is estimated to be from 10%-20%, with higher rates in higher altitudes and in Western countries. In a 2023 study of 844 patients, a significant proportion of individuals had darker skin phototypes, and further studies that elucidate prevalence in darker skin are needed.
The etiology of PMLE is not well understood. One theory is that UVR modifies antigens in the skin of PMLE patients to make them immunogenic. There are also data to suggest that PMLE involves a type IV delayed-type hypersensitivity reaction. The action spectrum for PMLE is UVA in most cases, but UVB and both UVA and UVB may also incite the response. Recent studies have shown that PMLE is associated with mutations in the NOD2 and TLR5 genes.
Although the condition frequently recurs, the tendency toward the development of PMLE and the severity of the eruption diminish with repeated sunlight exposure. This phenomenon is termed "hardening." As the summer proceeds, it has been observed that the incidence of new eruptions decreases. Prophylactic phototherapy supports this concept of hardening or tolerance.
Despite the variability of presentations, individual patients tend to experience the same clinical manifestations with each episode.
Codes
ICD10CM:
L56.4 – Polymorphous light eruption
SNOMEDCT:
238525001 – Polymorphous light eruption
L56.4 – Polymorphous light eruption
SNOMEDCT:
238525001 – Polymorphous light eruption
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:06/20/2023
Last Updated:07/18/2023
Last Updated:07/18/2023
 Patient Information for Polymorphous light eruption in Adult
Patient Information for Polymorphous light eruption in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today