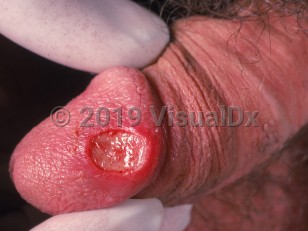
Primary syphilis - Anogenital in
See also in: Overview,Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Syphilis crisis in the United States: Syphilis and congenital syphilis cases have been surging nationwide, with an 80% increase in total syphilis cases between 2018 and 2022. Serologic testing is the primary means of diagnosing, staging, and managing syphilis. Testing should be done for any sexually active patient in whom syphilis is suspected or who has new, unexplained symptoms. Prompt diagnosis and treatment of syphilis can prevent systemic complications, including ocular involvement and permanent blindness.
Syphilis is a sexually transmitted infection (STI) caused by the spirochete bacterium Treponema pallidum. It is characterized by a chronic intermittent clinical course. Treponema pallidum is transmitted person to person via direct contact with a syphilis ulcer during vaginal, anal, or oral sex and may enter through skin or mucous membranes. Hence, the locations for syphilitic ulcers include the vagina, cervix, penis, anus, rectum, lips, hands, and inside of the mouth.
In the primary stage of syphilis, a painless ulceration or chancre typically appears about 21 days after initial infection, often preceded by a firm, painless papule. The chancre is easily seen on the frenulum or on the coronal sulcus of the penis but may hide under the foreskin. The entire genital area is susceptible, including the anus and inside the urethra. Chancres are typically asymptomatic. If secondary erosion or fissuring occurs, they may be painful. Other symptoms may include bloody stool and rectal pain.
Chancres vary in size from a few millimeters to several centimeters. They have an incubation period of 10-90 days (average 21 days). The chancre lasts 3-6 weeks and heals spontaneously.
Follmann balanitis refers to the rare variant of primary syphilis that presents with scattered erosions of the glans and foreskin. A primary chancre may be seen in association or may occur before it presents or after resolution.
All patients with primary syphilis will go on to develop secondary syphilis if the condition is left untreated. Secondary syphilis usually appears 3-10 weeks after the primary chancre and is characterized by a papulosquamous eruption and mucosal involvement, in some cases. Tertiary syphilis may appear months to years after secondary syphilis resolves and can involve the central nervous system (CNS), heart, bones, and skin.
Ocular screening (eg, slit lamp examination) is advised for patients with suspected or proven syphilis.
Per the US Centers for Disease Control and Prevention (CDC), the majority of reported male primary and secondary syphilis cases where sex of sex partner is known are among men who have sex with men. An increased incidence of syphilis is associated with HIV positivity.
Immunocompromised patient considerations: Genital ulcers caused by syphilis increase the risk of HIV transmission due to epithelial barrier compromise and increased numbers of macrophages and T-lymphocytes with HIV-specific receptors.
HIV infection can alter the clinical presentation of syphilis. Manifestations include multiple chancres, atypical cutaneous eruptions, increased severity of organ involvement (such as hepatitis and glomerulonephritis), and rapidly developing arteritis and neurosyphilis. Neurosyphilis can occur at any stage of syphilis.
Related topics: ocular syphilis, endemic syphilis
Syphilis is a sexually transmitted infection (STI) caused by the spirochete bacterium Treponema pallidum. It is characterized by a chronic intermittent clinical course. Treponema pallidum is transmitted person to person via direct contact with a syphilis ulcer during vaginal, anal, or oral sex and may enter through skin or mucous membranes. Hence, the locations for syphilitic ulcers include the vagina, cervix, penis, anus, rectum, lips, hands, and inside of the mouth.
In the primary stage of syphilis, a painless ulceration or chancre typically appears about 21 days after initial infection, often preceded by a firm, painless papule. The chancre is easily seen on the frenulum or on the coronal sulcus of the penis but may hide under the foreskin. The entire genital area is susceptible, including the anus and inside the urethra. Chancres are typically asymptomatic. If secondary erosion or fissuring occurs, they may be painful. Other symptoms may include bloody stool and rectal pain.
Chancres vary in size from a few millimeters to several centimeters. They have an incubation period of 10-90 days (average 21 days). The chancre lasts 3-6 weeks and heals spontaneously.
Follmann balanitis refers to the rare variant of primary syphilis that presents with scattered erosions of the glans and foreskin. A primary chancre may be seen in association or may occur before it presents or after resolution.
All patients with primary syphilis will go on to develop secondary syphilis if the condition is left untreated. Secondary syphilis usually appears 3-10 weeks after the primary chancre and is characterized by a papulosquamous eruption and mucosal involvement, in some cases. Tertiary syphilis may appear months to years after secondary syphilis resolves and can involve the central nervous system (CNS), heart, bones, and skin.
Ocular screening (eg, slit lamp examination) is advised for patients with suspected or proven syphilis.
Per the US Centers for Disease Control and Prevention (CDC), the majority of reported male primary and secondary syphilis cases where sex of sex partner is known are among men who have sex with men. An increased incidence of syphilis is associated with HIV positivity.
Immunocompromised patient considerations: Genital ulcers caused by syphilis increase the risk of HIV transmission due to epithelial barrier compromise and increased numbers of macrophages and T-lymphocytes with HIV-specific receptors.
HIV infection can alter the clinical presentation of syphilis. Manifestations include multiple chancres, atypical cutaneous eruptions, increased severity of organ involvement (such as hepatitis and glomerulonephritis), and rapidly developing arteritis and neurosyphilis. Neurosyphilis can occur at any stage of syphilis.
Related topics: ocular syphilis, endemic syphilis
Codes
ICD10CM:
A51.0 – Primary genital syphilis
SNOMEDCT:
266127002 – Primary syphilis
A51.0 – Primary genital syphilis
SNOMEDCT:
266127002 – Primary syphilis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:08/24/2020
Last Updated:04/03/2024
Last Updated:04/03/2024
 Patient Information for Primary syphilis - Anogenital in
Patient Information for Primary syphilis - Anogenital in
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Primary syphilis - Anogenital in
See also in: Overview,Oral Mucosal Lesion