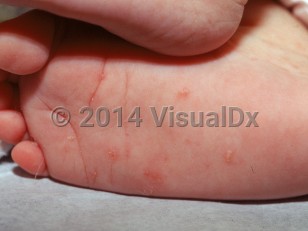
Scabies (pediatric) in Infant/Neonate
See also in: AnogenitalAlerts and Notices
Important News & Links
Synopsis

This summary discusses pediatric patients. Scabies in adults is addressed separately.
Scabies is a parasitic infestation of the epidermis. It is caused by the obligate human parasite Sarcoptes scabiei var hominis and is transmitted via direct skin-to-skin contact and rarely by fomites. Scabies affects all ethnic groups and socioeconomic levels. It is most common in young children, and the highest prevalence is seen in children younger than 2 years. It is extremely contagious, spreading between individuals who share close contact or living spaces. Frequent outbreaks occur in schools, group homes, and orphanages where direct contact with infested individuals is common. The most common predisposing factors are overcrowding, poverty, poor nutrition, and being undomiciled. Other predisposing conditions include immunocompromised status, HIV infection, and severe intellectual or physical disability.
Symptoms and signs typically develop approximately 3 weeks after the primary infestation. The most common clinical manifestation of scabies in infants is the development of pustules, vesicles, and crusting. The palms and soles, fingers, face, and scalp are most heavily involved. Secondary impetigo and eczematization are also common. The primary symptom of infestation is pruritus, and in young infants who have not developed a coordinated itch response, this may manifest as rubbing the head against a caregiver, irritability, insomnia, and poor feeding.
Crusted scabies (formerly known as Norwegian scabies) is a variant of scabies characterized by profuse proliferation of mites within the epidermis, with subsequent widespread scaly, crusted, or hyperkeratotic papules and plaques. Pruritus may be severe but is usually minimal or absent. It is mainly seen in immunocompromised individuals.
Scabies is a parasitic infestation of the epidermis. It is caused by the obligate human parasite Sarcoptes scabiei var hominis and is transmitted via direct skin-to-skin contact and rarely by fomites. Scabies affects all ethnic groups and socioeconomic levels. It is most common in young children, and the highest prevalence is seen in children younger than 2 years. It is extremely contagious, spreading between individuals who share close contact or living spaces. Frequent outbreaks occur in schools, group homes, and orphanages where direct contact with infested individuals is common. The most common predisposing factors are overcrowding, poverty, poor nutrition, and being undomiciled. Other predisposing conditions include immunocompromised status, HIV infection, and severe intellectual or physical disability.
Symptoms and signs typically develop approximately 3 weeks after the primary infestation. The most common clinical manifestation of scabies in infants is the development of pustules, vesicles, and crusting. The palms and soles, fingers, face, and scalp are most heavily involved. Secondary impetigo and eczematization are also common. The primary symptom of infestation is pruritus, and in young infants who have not developed a coordinated itch response, this may manifest as rubbing the head against a caregiver, irritability, insomnia, and poor feeding.
Crusted scabies (formerly known as Norwegian scabies) is a variant of scabies characterized by profuse proliferation of mites within the epidermis, with subsequent widespread scaly, crusted, or hyperkeratotic papules and plaques. Pruritus may be severe but is usually minimal or absent. It is mainly seen in immunocompromised individuals.
Codes
ICD10CM:
B86 – Scabies
SNOMEDCT:
128869009 – Infestation by Sarcoptes scabiei var hominis
B86 – Scabies
SNOMEDCT:
128869009 – Infestation by Sarcoptes scabiei var hominis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:02/15/2023
Last Updated:04/06/2023
Last Updated:04/06/2023
 Patient Information for Scabies (pediatric) in Infant/Neonate
Patient Information for Scabies (pediatric) in Infant/Neonate
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Scabies (pediatric) in Infant/Neonate
See also in: Anogenital