- Initial considerations in the setting of endocarditis do not differ from other emergency hemodynamic stabilization approaches.
- Obtain blood cultures early if endocarditis is suspected.
- Involve the cardiac surgery team as early as possible if surgical intervention may be warranted.
Endocarditis is a potentially life-threatening disease of the cardiac endothelium, most frequently involving the valves, caused by vegetations, infection, or both. Most cases of endocarditis are infectious, but it can also have noninfectious etiologies, such as in Libman-Sacks endocarditis where vegetations form secondary to autoimmune disease. Additionally, endocarditis can present as either acute or subacute disease and may be valvular or nonvalvular.
Endocarditis is a serious medical condition with an incidence rate of 15 per 100 000 people, an in-hospital mortality rate of around 20%, a 6-month mortality rate of around 30%, and a 1-year mortality rate approaching 40%. If surgery is indicated, early surgical intervention is associated with lower mortality. The incidence of endocarditis is increasing overall with more indwelling cardiovascular devices and increasing rates of intravenous (IV) drug use, which are major risk factors for this disease. Other risk factors include chronic hemodialysis, intravascular catheters, skin infections, recent dental procedures, poor dentition, prosthetic valve(s), age older than 60 years, male sex, congenital or acquired valvular heart disease, and prior infective endocarditis. Endocarditis should be considered in immunodeficient patients and patients with certain congenital or heritable heart malformations.
Community-acquired infection remains the most common cause of endocarditis, comprising up to 70% of cases, and is most commonly caused by oral, gastrointestinal (GI), and cutaneous bacteria. The most common bacterial cause in higher-income countries is Staphylococcus aureus (in up to 40% of cases).
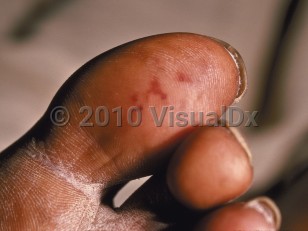
Signs and symptoms include a sudden onset of high fever, sepsis, or systemic complications, especially in the setting of a new heart murmur. Additionally, worsening of an old murmur, hematuria, and vascular embolic events should raise concern for endocarditis. Although there are classically taught pathognomonic signs and symptoms consistent with endocarditis, such as Janeway lesions, Roth spots, and splinter hemorrhages, these are found in a minority of patients, and their absence should not eliminate endocarditis from the differential.
The risk of developing prosthetic valve endocarditis is greatest during the initial 3 months after surgery, remains high for 6 months, and then falls gradually. Infection generally occurs with equal frequency on aortic and mitral sites as well as on mechanical and bioprosthetic devices during the first postoperative year. Afterward, bioprosthetic valves have a higher risk of infection due to age-related alterations in the valves' surfaces.
Libman-Sacks endocarditis is a noninfective cardiac valve disease that was initially described in patients with systemic lupus erythematosus (SLE). This form of endocarditis might occur in patients with antiphospholipid antibody syndrome. Vegetations on cardiac valves in Libman-Sacks endocarditis are composed primarily of inflammatory cells and fibrin clots. Endocarditis is presumed to be caused by autoimmunity against a cardiac valve with concurrent hypercoagulability. Patients are often asymptomatic but may be discovered after a cardioembolism causes ischemic injury, such as stroke or peripheral embolic disease. Libman-Sacks endocarditis is most frequently seen on the mitral and/or aortic valves and may cause valve dysfunction.