Potentially life-threatening emergency
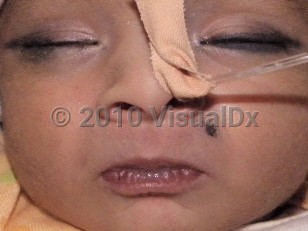
Tetanus neonatorum
Alerts and Notices
Important News & Links
Synopsis

Tetanus neonatorum is a severe clinical presentation of generalized tetanus in neonates. It is 1 of the 4 clinical patterns of tetanus (the other patterns being generalized tetanus, localized tetanus, and cephalic tetanus). All forms of tetanus are caused by the tetanus toxin produced by the bacterium Clostridium tetani. See tetanus for further discussion of other patterns.
Neonatal tetanus differs from the other clinical patterns of tetanus because it is the umbilical stump instead of a deep puncture wound that is inoculated by the bacterial spores. The umbilical stump acts as the portal of entry after contamination by nonsterile instruments or from the substances applied on it at birth that may include animal feces. In parts of the world where there are lower rates of maternal immunization against tetanus, where there is inadequate hygiene at the time of birth, and where there are cultural practices that lead to contamination of the umbilical stump, neonatal tetanus remains a significant cause of neonatal mortality.
The World Health Organization (WHO) initiated a program in 1999 to eliminate maternal and neonatal tetanus. As of December 2020, 12 of the 59 high-risk countries still have not reached elimination status: Afghanistan, Angola, Central African Republic, Guinea, Mali, Nigeria, Pakistan, Papua New Guinea, Somalia, South Sudan, Sudan, and Yemen.
Spores from C tetani are distributed worldwide in soil. Since continued exposure in the environment is expected, a robust vaccination program is necessary to prevent infections. Vaccination of women of childbearing age has been shown to be highly effective in preventing cases of neonatal tetanus. Improving hygiene at the time of birth with handwashing, clean handling of the cord, and application of topical antibiotics are also important, even if the strength of the evidence is poor so far.
In developed countries such as the United States, tetanus neonatorum is rare due to near universal vaccination (vaccination occurs in childhood with boosters as recommended by the Advisory Committee on Immunization Practices).
The WHO definition for a clinical case of tetanus neonatorum is "any neonate with normal ability to suck and cry during the first 2 days of life and who, between 3 and 28 days of age, cannot suck normally and becomes stiff or has spasms (ie, jerking of the muscles)."
The infant presents with diffuse rigidity, muscle spasms, trismus (lockjaw), apnea, and inability to suck. Patients may also suffer symptoms of autonomic dysfunction such as labile blood pressures. These symptoms are quite similar to adult patients with generalized tetanus, although the rate of disease progression is typically more rapid in neonatal tetanus.
The median onset of symptoms after birth is after 5-7 days, but ranges from 3-14 days, depending on the amount of spores soiling the cord.
The symptoms are severe for up to 4 weeks (the neonate will typically require intensive care during this period). After the acute illness, symptoms continue to improve over the following weeks. Mortality is high in neonatal tetanus. Many patients who survive will be left with permanent disabilities including developmental delay.
Neonatal tetanus differs from the other clinical patterns of tetanus because it is the umbilical stump instead of a deep puncture wound that is inoculated by the bacterial spores. The umbilical stump acts as the portal of entry after contamination by nonsterile instruments or from the substances applied on it at birth that may include animal feces. In parts of the world where there are lower rates of maternal immunization against tetanus, where there is inadequate hygiene at the time of birth, and where there are cultural practices that lead to contamination of the umbilical stump, neonatal tetanus remains a significant cause of neonatal mortality.
The World Health Organization (WHO) initiated a program in 1999 to eliminate maternal and neonatal tetanus. As of December 2020, 12 of the 59 high-risk countries still have not reached elimination status: Afghanistan, Angola, Central African Republic, Guinea, Mali, Nigeria, Pakistan, Papua New Guinea, Somalia, South Sudan, Sudan, and Yemen.
Spores from C tetani are distributed worldwide in soil. Since continued exposure in the environment is expected, a robust vaccination program is necessary to prevent infections. Vaccination of women of childbearing age has been shown to be highly effective in preventing cases of neonatal tetanus. Improving hygiene at the time of birth with handwashing, clean handling of the cord, and application of topical antibiotics are also important, even if the strength of the evidence is poor so far.
In developed countries such as the United States, tetanus neonatorum is rare due to near universal vaccination (vaccination occurs in childhood with boosters as recommended by the Advisory Committee on Immunization Practices).
The WHO definition for a clinical case of tetanus neonatorum is "any neonate with normal ability to suck and cry during the first 2 days of life and who, between 3 and 28 days of age, cannot suck normally and becomes stiff or has spasms (ie, jerking of the muscles)."
The infant presents with diffuse rigidity, muscle spasms, trismus (lockjaw), apnea, and inability to suck. Patients may also suffer symptoms of autonomic dysfunction such as labile blood pressures. These symptoms are quite similar to adult patients with generalized tetanus, although the rate of disease progression is typically more rapid in neonatal tetanus.
The median onset of symptoms after birth is after 5-7 days, but ranges from 3-14 days, depending on the amount of spores soiling the cord.
The symptoms are severe for up to 4 weeks (the neonate will typically require intensive care during this period). After the acute illness, symptoms continue to improve over the following weeks. Mortality is high in neonatal tetanus. Many patients who survive will be left with permanent disabilities including developmental delay.
Codes
ICD10CM:
A33 – Tetanus neonatorum
SNOMEDCT:
43424001 – Tetanus neonatorum
A33 – Tetanus neonatorum
SNOMEDCT:
43424001 – Tetanus neonatorum
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:04/25/2022
Last Updated:05/15/2022
Last Updated:05/15/2022