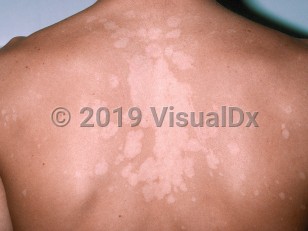
Tinea versicolor in Child
Alerts and Notices
Important News & Links
Synopsis

Tinea versicolor, also known as pityriasis versicolor, is a common, benign superficial fungal infection of the skin. Infective organisms are dimorphic yeast of the Malassezia genus. The yeast forms of these organisms are part of the normal skin flora; however, conversion to the filamentous form leads to the appearance of tinea versicolor.
Clinically, the infection manifests as macules, papules, patches, and plaques of varying pigmentation with fine scale. The disease typically occurs in a seborrheic distribution including the upper trunk and arms, neck, and face. The suprapubic skin is another site of predilection. The rash is rarely pruritic, and the primary concern is usually its appearance.
The distribution is worldwide, but the condition is most commonly found in tropical areas with high humidity and temperatures. Young adults and teenagers seem to be affected more frequently due to increased sebaceous gland activity.
Tinea versicolor is not contagious. Factors mediating its development include heat, humidity, oral contraceptives, corticosteroid use, and immune suppression. Individuals with oily skin or a positive family history may be more susceptible.
The disease typically begins during or just after the warmest months of the year. It may last from weeks to months. There are no associated systemic signs. This condition should be in the differential diagnosis of any hypopigmented or hyperpigmented macules or patches on the body.
Clinically, the infection manifests as macules, papules, patches, and plaques of varying pigmentation with fine scale. The disease typically occurs in a seborrheic distribution including the upper trunk and arms, neck, and face. The suprapubic skin is another site of predilection. The rash is rarely pruritic, and the primary concern is usually its appearance.
The distribution is worldwide, but the condition is most commonly found in tropical areas with high humidity and temperatures. Young adults and teenagers seem to be affected more frequently due to increased sebaceous gland activity.
Tinea versicolor is not contagious. Factors mediating its development include heat, humidity, oral contraceptives, corticosteroid use, and immune suppression. Individuals with oily skin or a positive family history may be more susceptible.
The disease typically begins during or just after the warmest months of the year. It may last from weeks to months. There are no associated systemic signs. This condition should be in the differential diagnosis of any hypopigmented or hyperpigmented macules or patches on the body.
Codes
ICD10CM:
B36.0 – Pityriasis versicolor
SNOMEDCT:
56454009 – Tinea versicolor
B36.0 – Pityriasis versicolor
SNOMEDCT:
56454009 – Tinea versicolor
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:06/20/2016
 Patient Information for Tinea versicolor in Child
Patient Information for Tinea versicolor in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today