The European Birt-Hogg-Dubé consortium proposed guidelines for the diagnosis as fulfilling either one major or two minor criteria.
Major criteria:
- At least five fibrofolliculomas or trichodiscomas, at least one histologically confirmed, of adult onset.
- Pathogenic FLCN germline mutation.
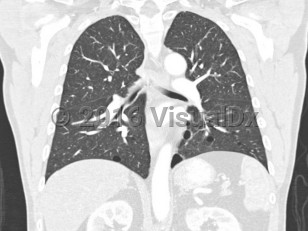
- Multiple lung cysts: bilateral basally located lung cysts with no other apparent cause, with or without spontaneous primary pneumothorax.
- Renal cancer: early onset (age younger than 50 years) or multifocal or bilateral renal cancer or renal cancer of mixed chromophobe and oncocytic histology.
- A first degree relative with BHD.
Approximately 80% of patients develop pulmonary cysts, which can be numerous and bilateral. They commonly affect the base of the lungs. They typically develop between the ages of 30 and 40 but have been described from ages 20-85. BHD patients are at 50-fold increased risk of spontaneous pneumothorax, with approximately 24% of those with pulmonary cysts developing spontaneous pneumothoraces at an average age of 38 years (range: 22-71 years). FLCN-mutation carriers have developed pneumothoraces as early as age 7.
Renal tumors occur in approximately 12%-34% of BHD patients at a mean age of 50.4 years (range: 30-70 years). Patients have a 7-fold increased risk of renal tumors compared to the general population. Renal tumors can be bilateral, unilateral, or multifocal. The most common types of renal tumors in this patient population are chromophobe tumors and hybrid chromophobe / oncocytic tumors; however, clear cell carcinoma, papillary carcinoma, and mixed-type carcinoma may also occur.