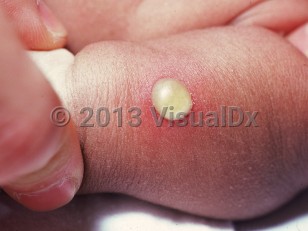
Bullous impetigo (pediatric) - Anogenital in
See also in: OverviewAlerts and Notices
Important News & Links
Synopsis

This summary discusses pediatric patients. Bullous impetigo in adults is addressed separately.
Bullous impetigo is a localized form of staphylococcal scalded skin syndrome caused by exfoliative toxins (A and B) released by (phage group II) Staphylococcus aureus. These toxins cleave desmoglein 1, resulting in superficial blisters locally at the site of infection. It is primarily seen in children, especially infants, who lack antibodies against exfoliative toxins, and only rarely occurs in teenagers or young adults. Infection is spread by direct contact with colonized or infected individuals. Staphylococcus aureus often colonizes the nares, umbilicus, nails, and eyes; approximately 5% of S aureus has exfoliative toxin.
Bullous impetigo initially presents as flaccid bullae, which then rupture, leaving round erosions that become crusted. Constitutional symptoms and fever are rare and mild, if they occur. The disease commonly affects the intertriginous areas, face, and extremities.
Outbreaks tend to occur during the summer months and in humid climates. Full resolution typically occurs within 2-6 weeks. Rare progression to staphylococcal scalded skin syndrome can occur.
In neonates, the infection often presents in the first 2 weeks of life. Sometimes, bullous impetigo may result in serious infections like osteomyelitis, septic arthritis, pneumonia, and septicemia.
Bullous impetigo is a localized form of staphylococcal scalded skin syndrome caused by exfoliative toxins (A and B) released by (phage group II) Staphylococcus aureus. These toxins cleave desmoglein 1, resulting in superficial blisters locally at the site of infection. It is primarily seen in children, especially infants, who lack antibodies against exfoliative toxins, and only rarely occurs in teenagers or young adults. Infection is spread by direct contact with colonized or infected individuals. Staphylococcus aureus often colonizes the nares, umbilicus, nails, and eyes; approximately 5% of S aureus has exfoliative toxin.
Bullous impetigo initially presents as flaccid bullae, which then rupture, leaving round erosions that become crusted. Constitutional symptoms and fever are rare and mild, if they occur. The disease commonly affects the intertriginous areas, face, and extremities.
Outbreaks tend to occur during the summer months and in humid climates. Full resolution typically occurs within 2-6 weeks. Rare progression to staphylococcal scalded skin syndrome can occur.
In neonates, the infection often presents in the first 2 weeks of life. Sometimes, bullous impetigo may result in serious infections like osteomyelitis, septic arthritis, pneumonia, and septicemia.
Codes
ICD10CM:
L01.03 – Bullous impetigo
SNOMEDCT:
399183005 – Impetigo bullosa
L01.03 – Bullous impetigo
SNOMEDCT:
399183005 – Impetigo bullosa
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:03/22/2022
Last Updated:05/05/2022
Last Updated:05/05/2022
 Patient Information for Bullous impetigo (pediatric) - Anogenital in
Patient Information for Bullous impetigo (pediatric) - Anogenital in
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Bullous impetigo (pediatric) - Anogenital in
See also in: Overview