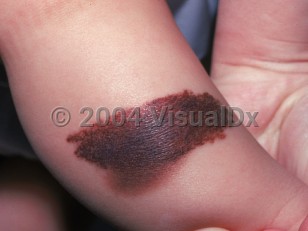
Congenital melanocytic nevus - Anogenital in
See also in: Overview,External and Internal Eye,Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

Congenital melanocytic nevus (CMN) is a benign nevus present at birth or within the first few weeks of life. CMNs are often flat and tan in color, initially resembling an irregular café au lait macule, but may change during the first few years of life and can vary tremendously in size. They are mostly on the trunk (~38%) or extremities (~48%) and less commonly on the head and neck (~14%). Most are elevated lesions that are primarily brown but may have variation in pigmentation including black, gray, and blue. Approximately 3% of patients have multiple CMNs. Compared with acquired nevi, CMNs have an earlier onset and are often larger with a more heterogeneous morphology.
One of the principal categorizations of CMNs is by size based on the projected maximal diameter of the CMN in adulthood. Different size cutoffs have been used with a recent proposed categorization including the categories of: small (< 1.5 cm), medium (M1: 1.5-10 cm, M2: > 10-20 cm), large (L1: > 20-30 cm, L2: > 30-40 cm), and giant (G1: > 40-60 cm, G2: > 60 cm). Most CMNs are less than 3-4 cm, with larger lesions being less common. CMNs have a slight female predominance (3:2) and are more common among patients of African and Japanese descent compared with individuals of Hispanic or Northern European descent.
CMNs have been associated with many benign lesions, the most common of which include café au lait macules and mucosal nevi.
CMNs have also been reported to have an increased risk for transformation to melanoma. The risk of melanoma is believed to correlate with CMN size. The incident rate of melanoma arising in small or medium CMNs is reported to be less than 1%. In one meta-analysis, melanoma was estimated to develop in approximately 2% of large CMNs (> 20 cm). Melanomas were diagnosed at a mean age of 12 years (range: birth to 58 years old), with 82% cutaneous and 13% visceral. Most cutaneous melanomas were located on the trunk (68%), and most of the melanoma-associated CMNs exceeded 40 cm in diameter (74%), with 94% of patients also having satellite nevi.
Large CMNs overlying limbs can be associated with atrophy of the subcutaneous tissue. Large CMNs over the head or axial skeleton should alert the physician to assess for neurocutaneous involvement (developmental delays, seizures, hydrocephalous, increased intracranial pressure).
Neurocutaneous melanosis is when a CMN is associated with neuromelanosis, a congenital error in ectodermal morphogenesis resulting in melanocytic proliferation within the leptomeninges and brain parenchyma. This most commonly occurs in larger CMNs. While not all patients are symptomatic, there can be diverse neurologic findings that typically present by 2 years of age.
CMN may also be associated with other syndromes such as Carney (pigmented skin lesions and atrial myxomas), LAMB (lentigines, atrial myxoma, mucocutaneous myxoma, blue nevi), NAME (nevi, atrial myxoma, myxoid neurofibromata, ephelides), neurocutaneous melanosis, premature aging syndrome, occult spinal dysraphism, and possibly neurofibromatosis type 1, and other malformation syndromes.
Related topic: Giant Congenital Nevus
One of the principal categorizations of CMNs is by size based on the projected maximal diameter of the CMN in adulthood. Different size cutoffs have been used with a recent proposed categorization including the categories of: small (< 1.5 cm), medium (M1: 1.5-10 cm, M2: > 10-20 cm), large (L1: > 20-30 cm, L2: > 30-40 cm), and giant (G1: > 40-60 cm, G2: > 60 cm). Most CMNs are less than 3-4 cm, with larger lesions being less common. CMNs have a slight female predominance (3:2) and are more common among patients of African and Japanese descent compared with individuals of Hispanic or Northern European descent.
CMNs have been associated with many benign lesions, the most common of which include café au lait macules and mucosal nevi.
CMNs have also been reported to have an increased risk for transformation to melanoma. The risk of melanoma is believed to correlate with CMN size. The incident rate of melanoma arising in small or medium CMNs is reported to be less than 1%. In one meta-analysis, melanoma was estimated to develop in approximately 2% of large CMNs (> 20 cm). Melanomas were diagnosed at a mean age of 12 years (range: birth to 58 years old), with 82% cutaneous and 13% visceral. Most cutaneous melanomas were located on the trunk (68%), and most of the melanoma-associated CMNs exceeded 40 cm in diameter (74%), with 94% of patients also having satellite nevi.
Large CMNs overlying limbs can be associated with atrophy of the subcutaneous tissue. Large CMNs over the head or axial skeleton should alert the physician to assess for neurocutaneous involvement (developmental delays, seizures, hydrocephalous, increased intracranial pressure).
Neurocutaneous melanosis is when a CMN is associated with neuromelanosis, a congenital error in ectodermal morphogenesis resulting in melanocytic proliferation within the leptomeninges and brain parenchyma. This most commonly occurs in larger CMNs. While not all patients are symptomatic, there can be diverse neurologic findings that typically present by 2 years of age.
CMN may also be associated with other syndromes such as Carney (pigmented skin lesions and atrial myxomas), LAMB (lentigines, atrial myxoma, mucocutaneous myxoma, blue nevi), NAME (nevi, atrial myxoma, myxoid neurofibromata, ephelides), neurocutaneous melanosis, premature aging syndrome, occult spinal dysraphism, and possibly neurofibromatosis type 1, and other malformation syndromes.
Related topic: Giant Congenital Nevus
Codes
ICD10CM:
D22.9 – Melanocytic nevi, unspecified
SNOMEDCT:
398696001 – Congenital melanocytic nevus
D22.9 – Melanocytic nevi, unspecified
SNOMEDCT:
398696001 – Congenital melanocytic nevus
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:09/04/2018
 Patient Information for Congenital melanocytic nevus - Anogenital in
Patient Information for Congenital melanocytic nevus - Anogenital in
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Congenital melanocytic nevus - Anogenital in
See also in: Overview,External and Internal Eye,Hair and Scalp