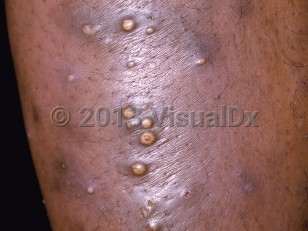
Furunculosis in Adult
See also in: Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

Furuncles (boils) are cutaneous abscesses associated with hair follicles. Carbuncles are a continuous collection of furuncles. By definition, furuncles are of infectious etiology, with the most common causative agent being Staphylococcus aureus (either methicillin-sensitive [MSSA] or methicillin-resistant [MRSA]). The infecting strain of Staphylococcus is usually colonizing the nares, umbilicus, or perineum. Furunculosis most commonly affects adolescents and young adults and is rarely seen in childhood. It more commonly affects males. Predisposing factors include Staphylococcus carriage, friction, malnutrition, poor hygiene, possibly diabetes, hyper-IgE syndrome, and human immunodeficiency virus (HIV) infection.
Clinically, furuncles are painful (particularly when in the nose or ear canal). They often appear in crops. Patients may describe purulent drainage. They usually occur on the face, neck, axillae, buttocks, thighs, and perineum. When on the central face, cavernous sinus thrombosis is a rare complication. Lesions may continue to develop for months to years, but individual lesions often heal spontaneously within 2-3 weeks.
MRSA first emerged as an important nosocomial pathogen in the 1960s. In more recent years, community-acquired outbreaks of MRSA (CA-MRSA) have been described increasingly among healthy individuals lacking the traditional risk factors for such infections (eg, IV drug use, incarceration, participation in contact sports). These strains have a propensity for causing abscesses, furunculosis, and folliculitis and have a unique antibiotic susceptibility profile from health care-associated strains of MRSA.
Immunocompromised patients have a significantly increased risk of developing both MSSA and MRSA furunculosis. HIV-infected patients are approximately 20 times more likely to develop skin and soft tissues infections caused by MRSA. Risk factors for MRSA infection in this population are low current CD4 cell count, recent beta-lactam antibiotic use, and high-risk sexual activity.
Clinically, furuncles are painful (particularly when in the nose or ear canal). They often appear in crops. Patients may describe purulent drainage. They usually occur on the face, neck, axillae, buttocks, thighs, and perineum. When on the central face, cavernous sinus thrombosis is a rare complication. Lesions may continue to develop for months to years, but individual lesions often heal spontaneously within 2-3 weeks.
MRSA first emerged as an important nosocomial pathogen in the 1960s. In more recent years, community-acquired outbreaks of MRSA (CA-MRSA) have been described increasingly among healthy individuals lacking the traditional risk factors for such infections (eg, IV drug use, incarceration, participation in contact sports). These strains have a propensity for causing abscesses, furunculosis, and folliculitis and have a unique antibiotic susceptibility profile from health care-associated strains of MRSA.
Immunocompromised patients have a significantly increased risk of developing both MSSA and MRSA furunculosis. HIV-infected patients are approximately 20 times more likely to develop skin and soft tissues infections caused by MRSA. Risk factors for MRSA infection in this population are low current CD4 cell count, recent beta-lactam antibiotic use, and high-risk sexual activity.
Codes
ICD10CM:
L02.92 – Furuncle, unspecified
SNOMEDCT:
416675009 – Furuncle
L02.92 – Furuncle, unspecified
SNOMEDCT:
416675009 – Furuncle
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:03/22/2018
Last Updated:03/22/2018
Last Updated:03/22/2018
 Patient Information for Furunculosis in Adult
Patient Information for Furunculosis in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Furunculosis in Adult
See also in: Hair and Scalp