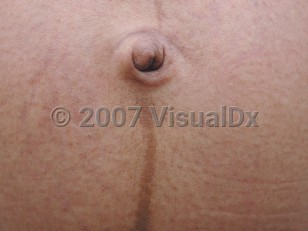
Linea nigra
Alerts and Notices
Important News & Links
Synopsis

Linea nigra (Latin for "black line"), also known as linea gravidarum, is a linear midline band of macular hyperpigmentation that runs vertically from the pubis to the xiphoid process. This entity is much more common in individuals with darker skin phototypes. It is most commonly seen in pregnant individuals, particularly those with darker skin phototypes.
Linea nigra is thought to be a consequence of increased production of melanin secondary to increased circulating levels of estrogen, progesterone, and melanocyte stimulating hormone (MSH) in pregnancy. Upregulation by human placenta lipids of tyrosinase has also been hypothesized to play a role. In 90% of pregnant individuals, hyperpigmentation of some type is seen, including darkening of the areolae, ephelides, scars, or melasma. Women with lighter skin phototypes develop hyperpigmentation less often than women with darker pigmentation. Linea nigra tends to appear around the second or third trimester. After birth, the line fades over time, but it may never disappear entirely.
In a population-based study of Nigerians, linea nigra was found to be present in both male and female patients. For males, incidence peaked at 40% in the 11- to 15-year-old age group, whereas in females, incidence was highest in the 16- to 30-year-old group, in which 85% were affected. Pregnant individuals were 60 times more likely than nonpregnant individuals to have linea nigra. In males, an increased incidence has been noted in patients with prostate cancer and benign prostatic hypertrophy. Its use as a screening tool for prostate cancer has been suggested, but it was not found to be a sensitive marker in one study.
Related topic: linea nigra in newborn
Linea nigra is thought to be a consequence of increased production of melanin secondary to increased circulating levels of estrogen, progesterone, and melanocyte stimulating hormone (MSH) in pregnancy. Upregulation by human placenta lipids of tyrosinase has also been hypothesized to play a role. In 90% of pregnant individuals, hyperpigmentation of some type is seen, including darkening of the areolae, ephelides, scars, or melasma. Women with lighter skin phototypes develop hyperpigmentation less often than women with darker pigmentation. Linea nigra tends to appear around the second or third trimester. After birth, the line fades over time, but it may never disappear entirely.
In a population-based study of Nigerians, linea nigra was found to be present in both male and female patients. For males, incidence peaked at 40% in the 11- to 15-year-old age group, whereas in females, incidence was highest in the 16- to 30-year-old group, in which 85% were affected. Pregnant individuals were 60 times more likely than nonpregnant individuals to have linea nigra. In males, an increased incidence has been noted in patients with prostate cancer and benign prostatic hypertrophy. Its use as a screening tool for prostate cancer has been suggested, but it was not found to be a sensitive marker in one study.
Related topic: linea nigra in newborn
Codes
ICD10CM:
L81.8 – Other specified disorders of pigmentation
O26.90 – Pregnancy related conditions, unspecified, unspecified trimester
SNOMEDCT:
90751002 – Linea nigra
L81.8 – Other specified disorders of pigmentation
O26.90 – Pregnancy related conditions, unspecified, unspecified trimester
SNOMEDCT:
90751002 – Linea nigra
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:08/11/2020
Last Updated:08/12/2021
Last Updated:08/12/2021
 Patient Information for Linea nigra
Patient Information for Linea nigra
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today