Infection occurs via airborne fungal spores found ubiquitously in dust, soil, and decaying organic materials that are inhaled through the nasopharynx entering into the lungs, sinuses, and gastrointestinal tract. The spores convert into hyphae upon invasion into human tissue, leading to subsequent angioinvasion and tissue necrosis.
The 5 major types of mucormycosis are:
- Rhino-orbital-cerebral disease – Patients present with unilateral facial pain, headaches, fever, nasal or sinus congestion and discharge, and black, necrotic ulcerations, usually involving the palate. Infection can erode locally and spread to the cavernous sinus, the internal carotid artery, and the brain. Orbital involvement can lead to orbital cellulitis, ophthalmoplegia, and multiple cranial nerve palsies, with a potential for permanent residual effects such as blindness and cranial nerve defects occurring up to 70% of the time. These patients may present with only a central retinal artery occlusion.
- Pulmonary disease – In the immunocompromised host, this can be insidiously and minimally symptomatic, often identified incidentally by chest CT or presenting with isolated fevers unresponsive to antibiotics. Some patients may develop cough, dyspnea, and unremitting fever despite broad-spectrum antibiotics. Hemoptysis occurs as a result of tissue necrosis and angio-invasion and, rarely, can be fatal. Physical examination findings are nonspecific and can include tachypnea, crackles, decreased breath sounds, and wheezing, although often the lung examination is normal.
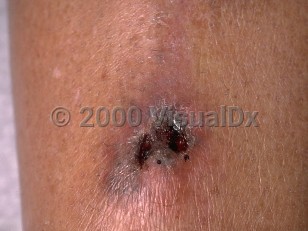
- Cutaneous disease – This form of mucormycosis may be primary or secondary. Primary infection may be associated with direct inoculation from trauma, burns, and surgical wounds. The affected tissue becomes inflamed, followed by subsequent necrosis. Secondary cutaneous mucormycosis occurs from hematogenous spread.
- Gastrointestinal disease – This is the most common form of mucormycosis in newborns. It is also seen in extreme cases of malnutrition or immunosuppression. It is believed to occur via direct ingestion of spores. Clinical findings may include feeding intolerance, fever, vomiting, diarrhea, abdominal distention, and gastrointestinal bleeding.
- Disseminated disease – This most commonly occurs following pulmonary mucormycosis, although it could be a result of any subtype. The brain is the most susceptible to infection, followed by the spleen, heart, skin, and other organs.
Pediatric patients with uncontrolled diabetes, particularly diabetic ketoacidosis, are predisposed to mucormycosis. These fungi have ketone reductase that allows them to thrive in high glucose, acidic environments. Additionally, acidosis decreases macrophage effectiveness, allowing rapid spread along injured blood vessels. Immunocompromised patients with cancer (especially lymphoma and leukemia), neutropenia, AIDS, malnutrition, or extensive burns, and patients who have had chemotherapy treatment, solid organ transplant, hematopoietic cell transplant, or chronic or high-dose steroid use are all susceptible to mucormycosis. Patients with iron overload being treated with deferoxamine are also at increased risk.
Neonates and patients with severe prematurity who are naturally immunocompromised from birth are also at high risk for mucormycosis. Premature infants often have other predisposing factors, such as immature skin barrier function, malnutrition, steroid treatment, hyperglycemia, acidosis, and broad-spectrum antibiotic use. When the gastrointestinal tract of neonates is involved, mucormycosis presents similarly to necrotizing enterocolitis. The fungus most often affects the colon, stomach, ileum, and appendix.