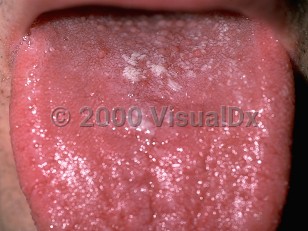
Oral candidiasis in Infant/Neonate
See also in: Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Transmission of infection occurs either at the time of delivery during passage through the vaginal canal or after delivery during handling or breastfeeding by the mother. Neonates that become infected at the time of delivery usually present with symptoms between 2 and 4 weeks of age. Infection later on in infancy can result from repeated use of antibiotics or occur in infants with human immunodeficiency virus (HIV) infection or a primary immunodeficiency syndrome.
Oral candidiasis appears in a number of clinical forms. The most common form is the pseudomembranous variety: white plaque formation typically appears on the tongue, lips, inner surface of the cheeks, and palate and can leave behind punctate bleeding and patches of reddened mucosa when scraped.
Candida at the corners of the mouth is known as angular cheilitis or perlèche. Crusting, small ulcers, or fissures can be present at the angles of the mouth.
The infant may be symptomless or may be generally irritable and show a decreased willingness to feed.
Related topics: Neonatal candidiasis, Diaper dermatitis candidiasis, Angular cheilitis, Congenital candidiasis
Codes
B37.0 – Candidal stomatitis
SNOMEDCT:
79740000 – Oral candidiasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:10/05/2017
 Patient Information for Oral candidiasis in Infant/Neonate
Patient Information for Oral candidiasis in Infant/Neonate- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient