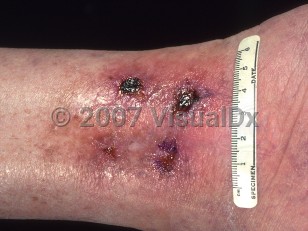
Ischemic ulcer
Alerts and Notices
Important News & Links
Synopsis

Ischemic (or arterial) ulcers are a type of vascular ulcer that occurs when there is inadequate blood supply to the skin. They are most frequently caused by progressive atherosclerosis (peripheral vascular disease) or arterial embolization. They predominantly involve the feet but, occasionally, can be seen with upper extremity occlusive disease such as thoracic outlet syndrome or Raynaud phenomenon.
Ischemic ulcers are often chronic in nature and are characteristically quite painful relative to other types of ulcers. Their occurrence may be precipitated by seemingly trivial trauma or localized pressure. The incidence of ischemic ulcers increases with advancing age; older individuals are also more likely to exhibit ulcers of mixed etiology. Patients with ischemic ulcers due to peripheral vascular disease will often give a history of claudication. Risk factors for the development of these ulcers include diabetes mellitus, smoking, hyperlipidemia, obesity, rheumatoid arthritis, a history of coronary artery disease, and hypertension. Martorell ulcer occurs in the setting of poorly controlled hypertension. Many patients have associated diabetes mellitus. Typically, there is an intensely painful ulcer on the inferior calf or over the Achilles tendon. Ischemia is thought to be a factor in its development.
Critical limb ischemia (CLI) is defined by the presence of longer than 2 weeks of limb pain at rest from ischemia, tissue loss due to ischemia, or ischemic ulceration. Clinicians of all types must be aware of the need for rapid revascularization, modifications in medical therapy, and wound care to minimize loss of limbs and loss of life in these patients.
Ischemic ulcers are often chronic in nature and are characteristically quite painful relative to other types of ulcers. Their occurrence may be precipitated by seemingly trivial trauma or localized pressure. The incidence of ischemic ulcers increases with advancing age; older individuals are also more likely to exhibit ulcers of mixed etiology. Patients with ischemic ulcers due to peripheral vascular disease will often give a history of claudication. Risk factors for the development of these ulcers include diabetes mellitus, smoking, hyperlipidemia, obesity, rheumatoid arthritis, a history of coronary artery disease, and hypertension. Martorell ulcer occurs in the setting of poorly controlled hypertension. Many patients have associated diabetes mellitus. Typically, there is an intensely painful ulcer on the inferior calf or over the Achilles tendon. Ischemia is thought to be a factor in its development.
Critical limb ischemia (CLI) is defined by the presence of longer than 2 weeks of limb pain at rest from ischemia, tissue loss due to ischemia, or ischemic ulceration. Clinicians of all types must be aware of the need for rapid revascularization, modifications in medical therapy, and wound care to minimize loss of limbs and loss of life in these patients.
Codes
ICD10CM:
I83.009 – Varicose veins of unspecified lower extremity with ulcer of unspecified site
SNOMEDCT:
13954005 – Ischemic ulcer
I83.009 – Varicose veins of unspecified lower extremity with ulcer of unspecified site
SNOMEDCT:
13954005 – Ischemic ulcer
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:05/12/2019
 Patient Information for Ischemic ulcer
Patient Information for Ischemic ulcer
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today