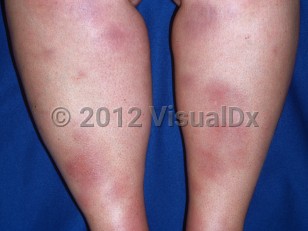
The eruption persists for 3-6 weeks and spontaneously regresses without ulceration, scarring, or atrophy.
EN occurs in boys and girls in equal proportions before puberty (it rarely occurs before age 2); however, after puberty, females are more frequently affected, as in the adult population. Recurrences with reappearance of the precipitating factor(s) are reported.
More commonly associated infections:
- Streptococcus infection, especially pharyngitis
- Mycoplasma
- Upper respiratory viruses (eg, EBV)
- Mycobacteria (tuberculosis [TB] and atypical)
- Coccidioidomycosis in endemic areas
- Yersinia, Shigella, Campylobacter, Salmonella sp gastroenteritis
- Cat-scratch disease, Chlamydia, syphilis, pertussis, leprosy, and numerous other bacterial infections
- Hepatitis B, HIV
- Blastomycosis, histoplasmosis, sporotrichosis, Giardia
- Sarcoidosis
- Inflammatory bowel disease
- Behçet disease
Drugs:
- Oral contraceptives, sulfonamides, penicillins, cephalosporins, macrolide antibiotics



 Patient Information for
Patient Information for